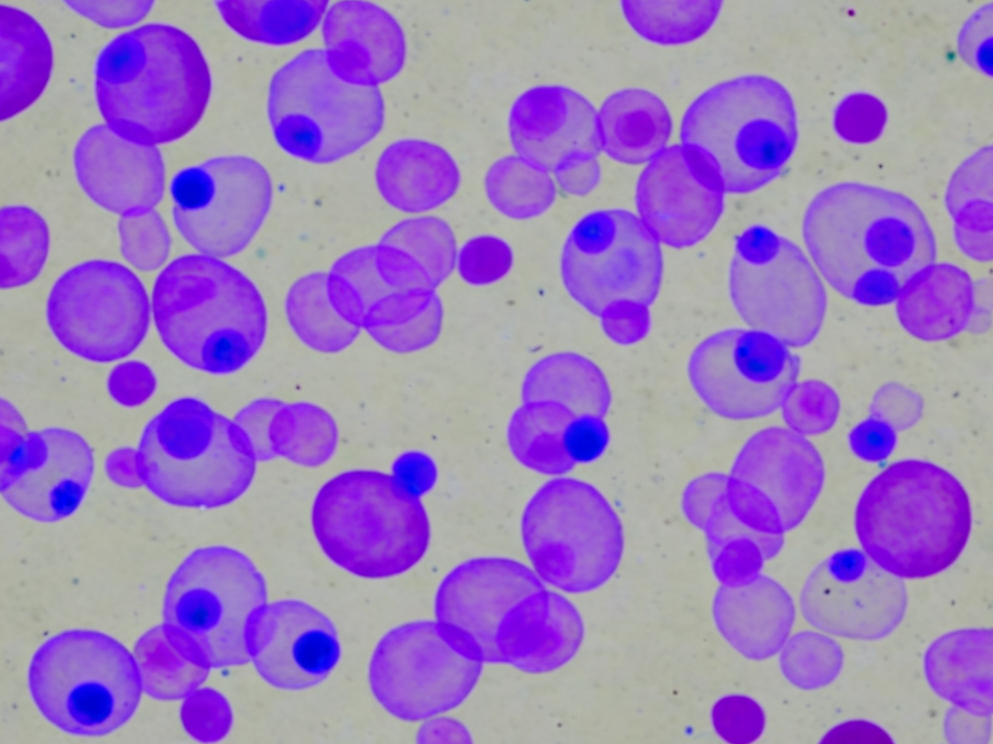
NALM-6 Cell Line: From B-ALL Pathology to Dual-Reporter Models
Introduction:
B-cell Acute Lymphoblastic Leukemia (B-ALL) remains a leading cause of cancer-related mortality in pediatric and young adult populations. While conventional chemotherapy induces remission in many patients, residual disease in sanctuary sites like the central nervous system (CNS) often leads to relapse. The NALM-6 cell line, established from a patient with relapsed B-ALL, has long served as a standard model for studying precursor B-cell leukemia biology. With the rise of precision medicine, particularly CAR-T therapy, the demand for visualizable in vivo models has surged. The engineered NALM-6-luc-gfp cell line, integrating bioluminescence and fluorescence, enables cross-scale tracing from single-cell analysis to whole-body imaging. This article details the fundamental biological characteristics of NALM-6 and explores the translational value of its dual-reporter derivative.
Origin and Background: Representative of Relapsed Pre-B ALL
The NALM-6 cell line was established in 1976 from the peripheral blood of a 19-year-old male experiencing a relapse of acute lymphoblastic leukemia. Originally classified as "non-T, non-B" leukemia in early immunotyping, subsequent molecular studies confirmed its lineage as precursor B-cell (Pre-B cell).
This cell line retains the highly aggressive characteristics of the clinical relapse case. In in vitro culture, NALM-6 exhibits typical single-cell suspension growth with a short doubling time (approximately 24-36 hours). Karyotypic analysis reveals a t(5;12)(q33;p13) translocation, involving the fusion of ETV6 and PDGFRB genes. Understanding this genetic background is crucial for studying sensitivity to specific kinase inhibitors. As a donor for human xenograft models, NALM-6 demonstrates a high engraftment rate in immunodeficient mice, authentically simulating the malignant proliferation of leukemic cells in the bone marrow and peripheral blood.
With stable growth kinetics and a clean background, the NALM-6 cell line is the premier choice for building reproducible B-ALL drug screening platforms. Shop now>>
The dominance of NALM-6 in immuno-oncology is largely attributed to its stable antigen expression profile. Flow cytometric analysis indicates that NALM-6 cells highly express CD19, CD10, and HLA-DR, while lacking surface immunoglobulin (sIg).
CD19 is the most successful target for Chimeric Antigen Receptor T-cell (CAR-T) therapy, and its expression abundance directly impacts CAR-T recognition and killing efficacy. Due to its uniform CD19 antigen density and expression levels comparable to clinical samples, NALM-6 is recognized as the "gold standard" target cell for evaluating CD19-CAR-T function. Researchers utilize this model to assess cytotoxicity, cytokine release (e.g., IFN-γ), and antigen escape mechanisms. Compared to other B-ALL cell lines like Raji or Daudi, NALM-6 also shows sensitivity to Bispecific T-cell Engager (BiTE) agents, such as Blinatumomab.
Dual-Reporter Principle: Construction Logic of NALM-6-luc-gfp
To overcome the limitations of traditional flow cytometry in monitoring real-time in vivo tumor distribution, researchers constructed the NALM-6-luc-gfp derivative. Through lentiviral transduction, genes encoding Firefly Luciferase and Green Fluorescent Protein (GFP) were stably integrated into the genome.
This dual-reporter system offers complementary experimental advantages:
Luciferase (Macroscopic Imaging): In in vivo experiments, injecting the substrate D-Luciferin allows for the detection of bioluminescent signals using IVIS imaging systems. The Photon Flux correlates linearly with tumor burden, enabling researchers to longitudinally monitor disease progression over weeks without sacrificing mice.
GFP (Microscopic Analysis): In in vitro experiments or during terminal dissection, the green fluorescent signal of GFP allows for precise differentiation of tumor cells from murine stromal cells via flow cytometry without additional antibody staining. This is particularly critical for analyzing Minimal Residual Disease (MRD) within the bone marrow microenvironment.
NALM-6-luc-gfp integrates Luc and GFP dual reporters, allowing one cell line to satisfy the full workflow from in vitro flow cytometry to in vivo imaging. Order now>>
Model Value: Central Nervous System (CNS) Infiltration Research
The unique application value of NALM-6-luc-gfp lies in its significant neurotropism. Clinically, CNS leukemia is a major cause of treatment failure because many chemotherapeutic agents cannot effectively cross the Blood-Brain Barrier (BBB).
When implanted into NSG or NOD SCID mice via tail vein injection, NALM-6-luc-gfp not only colonizes the bone marrow and spleen but also spontaneously migrates across the BBB, infiltrating the meninges and brain parenchyma. In bioluminescence images, this manifests as strong signal accumulation in the cranial region. This characteristic makes the model an ideal platform for screening small molecule inhibitors capable of penetrating the BBB or evaluating the CNS safety of novel CAR-T cells. By comparing the ratio of systemic to cranial signals, researchers can quantify the specific clearance capability of drugs against CNS lesions, a feat unachievable by most solid tumor models.
References
[1]Hurwitz, R., et al. (1979). Characterization of a leukemic cell line of the pre-B phenotype. International Journal of Cancer, 23(2), 174-180.
[2]Barrett, D. M., et al. (2011). Noninvasive bioluminescent imaging of primary patient acute lymphoblastic leukemia: a strategy for preclinical modeling. Blood, 118(15), e112-e117.
[3]Brentjens, R. J., et al. (2013). CD19-targeted T cells rapidly induce molecular remissions in adults with chemotherapy-refractory acute lymphoblastic leukemia. Science Translational Medicine, 5(177), 177ra38.
[4]Ebinger, S., et al. (2016). Characterization of the niche in the bone marrow of leukemic cells. Nature Medicine, 22(11), 1240-1250.

